
(305) 442-0066
Hialeah Office
North Miami Office
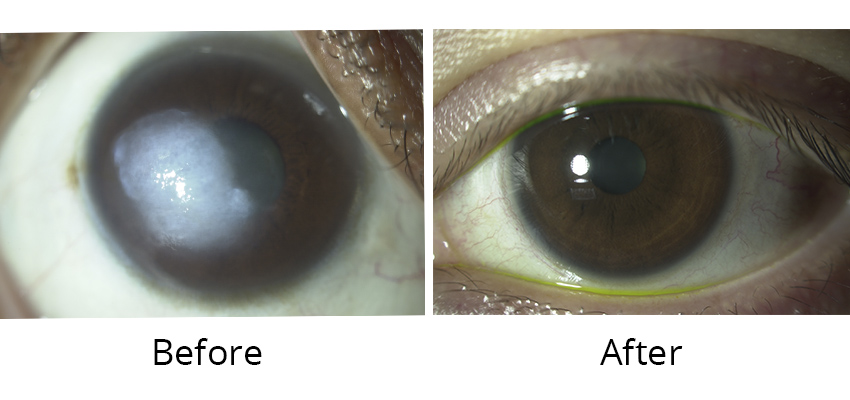
If the whole thickness of the cornea is affected and irreversibly cloudy, a full thickness transplant (penetrating keratoplasty) may be necessary to improve your vision. In some cases however, most of the cornea is healthy, but vision is affected only by the innermost layer of cells of the cornea (endothelial cells). The main reasons to have endothelial cell dysfunction are Fuchs Endothelial Corneal Dystrophy or after previous ocular surgery.
When this occurs we do not necessarily need to remove the entire cornea. A small incision is made on the side of your eye and only the unhealthy endothelial layer is removed. A layer of healthy endothelial cells from a donor is then inserted through this small incision and the cells are held in position by an air bubble injected into the eye. Because only a small incision is made in the eye, visual recovery is usually much quicker than with a full thickness transplant
Descemet’s Stripping Automated Endothelial Keratoplasty (DSAEK) vs Descemet’s Membrane Endothelial Keratoplasty (DMEK)
In DSAEK the endothelial cells are transplanted with a small sliver of stroma (middle layer of the cornea). The sliver of stroma can produce interface abnormalities between the donor and host potentially causing subtle disturbances in the quality of vision. The incision used in DSAEK is about 4.5mm and the final visual recovery takes about 3 months.
In DMEK the endothelial cells are transplanted without any stroma. Because there are no interface abnormalities DMEK can produce better quality vision. The incision is smaller (~2.5mm) than DSAEK and the final visual recovery takes about 1-2 months. Since there is a smaller amount of tissue transplanted the likelihood of corneal transplant rejection is lower in DMEK when compared to DSAEK.
In general DMEK is recommended when the eye anatomy is normal and organized. When patients have had several surgeries and there are abnormalities with the anatomy of the eye DMEK may not be possible and DSAEK may be preferred. Our specialists are well versed and experienced with both procedures and can recommend what is best for your specific needs.

2441 SW 37th Avenue
Miami, FL 33145
(305) 442-0066

202 E 49th Street
Hialeah, FL 33013
(305) 442-0066

2050 NE 163rd Street North
Miami Beach, FL 33162
Direct Line (786) 708-8372